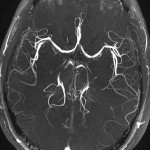
 Coronary CT angiography may be better than stress testing alone as a diagnostic tool for patients presenting with chest pain, according to the SCOT-HEART investigators.
Coronary CT angiography may be better than stress testing alone as a diagnostic tool for patients presenting with chest pain, according to the SCOT-HEART investigators.
Subsequent invasive angiography was less likely to show normal coronary arteries in patients diagnosed with coronary CT angiography results in lieu of stress testing data (0.96% versus 2.70% with stress testing, hazard ratio 0.39, 95% confidence interval 0.23-0.68). This group was also more likely to have confirmed obstructive coronary artery disease (CAD, 13.65% versus 11.10%, HR 1.29, 95% CI 1.08-1.55).
In addition, coronary CT angiography led to more use of preventive therapies (13.65% versus 3.57%, HR 4.03, 95% CI 3.12-5.20), David E. Newby, MD, of University of Edinburgh in the U.K., and colleagues reported online in the Journal of the American College of Cardiology.
Following-up 50 days after imaging, which was the median time for starting preventive drugs, the myocardial infarction rate in coronary CT angiography patients was half that seen in the control group (0.82% versus 1.64%, HR 0.50, 95% CI 0.28-0.88).
“We believe this reduction in events is consistent with the anticipated effect size attributable to initiation of preventive therapies together with potential benefits from lifestyle modification and coronary revascularization,” Newby and colleagues wrote.
“This suggests better use of invasive angiography, especially as the rate of coronary revascularization was high in those for whom coronary CT angiography had changed the initial diagnosis and suggested the presence of obstructive disease,” they wrote.
James K. Min, MD, of Weill Cornell Medical College in New York, and colleagues deemed the SCOT-HEART results the “highest-quality evidence to date for the comparative benefit of coronary CT angiography over standard-of-care approaches.”
“Not only may coronary CT angiography be considered a reasonable alternative to stress testing for initial diagnostic CAD evaluation, but it may actually be preferred,” they wrote in an accompanying editorial.
Coronary CT angiography now offers non-invasive fractional flow reserve measurements and thus may become “the oft-discussed ‘one-stop shop’ of coronary evaluation,” according to Min and colleagues.
Newby’s group concluded that “given the potentially greater hazards and costs of invasive angiography, our findings indicate that coronary CT angiography is as an effective and readily applicable gatekeeper for the conduct of invasive coronary angiography.”
The SCOT-HEART substudy included 4,146 patients who were randomized to receive standard care with or without coronary CT angiography.
Cumulative costs were higher in the CT group, with a mean difference of $462 at 6 months. The added expenses were directly attributable to the cost of coronary CT angiography itself, the investigators suggested, as downstream costs were the same between groups.
Min’s group noted that the earlier PROMISE trial had failed to show superiority for coronary CT angiography. That, they suggested, was due to “a follow-up period too short to enable realization of the salutary effects of preventive therapy, particularly in the trial’s population with a low prevalence of CAD.”
They argued that there is a gradient to CAD, which gives CT angiography an edge over stress testing.
“The ability to identify, quantify, and characterize atherosclerosis may be a distinguishing feature of coronary CT angiography that allows transcending beyond traditional lumen-based CAD assessments,” the editorialists wrote.
Newby and colleagues acknowledged that they were limited to a modest number of events in their study group of over 4,000 patients. “The majority of subjects had no or minimal CAD and therefore were not at risk,” they wrote, adding that longer-term study is underway to accrue more analyzable events.
Regardless, they concluded that “in patients with suspected angina due to coronary heart disease, coronary CT angiography leads to more appropriate use of invasive angiography and alterations in preventative therapies that were associated with a halving of fatal and non-fatal myocardial infarction.”